May 27, 2025
Alcohol and Heart Health: The Rise of AI in Addiction Treatment
Alcohol quietly harms the heart over time, raising blood pressure, weakening heart muscles, and increasing the risk of failure, even at so‑called “moderate” levels of drinking. With AI‑powered diagnostics, wearables, and personalized support, Helius Wellness helps detect risks early and guide smarter, more effective addiction treatment for long‑term heart health.
Author:
Paresh Masani
Though adults are usually the focus when we talk about heart disease, children can also face serious heart conditions. Childhood heart problems are rare, and congenital heart defects (CHD) often come to mind first. But cardiomyopathy is another serious condition that affects children.
Cardiomyopathy impacts the heart muscle, making it harder for the heart to pump blood properly. While it may not be as commonly discussed as CHD, it can have serious consequences for growth, development, and overall well-being. The challenge is that many families do not realize that young children may also face such conditions, which means diagnosis is often delayed.
By spreading awareness, offering clear information, and supporting parents with the right resources, we can help ensure children with cardiomyopathy receive care at the earliest stage possible. Early conversations about this condition open the door to better health outcomes and stronger support systems for families.
What is Cardiomyopathy in Children?
Cardiomyopathy is a disease of the heart muscle that reduces its ability to pump blood efficiently. Over time, this weakness or stiffness in the heart muscle can lead to heart failure, life-threatening arrhythmias, or even sudden cardiac arrest.
Unlike adult heart disease, which is often linked to lifestyle factors like smoking, obesity, or diabetes, cardiomyopathy in children is more often associated with genetic factors, infections, or underlying medical conditions.
Why Awareness of Cardiomyopathies is So Important?
Unlike congenital heart defects (CHD), which are often detected soon after birth, cardiomyopathy can develop months or even years later. This makes it trickier to spot, and many children don’t show obvious symptoms until the condition has progressed.
Reasons awareness is important:
- Silent progression: A child may appear healthy but still have underlying heart muscle weakness.
- Misdiagnosis risk: Fatigue, poor appetite, or fainting might be mistaken for minor health issues or even “laziness.
- High-risk outcomes: Cardiomyopathy is a leading cause of sudden cardiac death in young athletes. Many tragic incidents reported globally, including in India, involve children collapsing during school sports.
- Better prognosis with early care: When diagnosed early, many children can manage the disease with medication and lifestyle changes, avoiding severe complications.
Imagine a 10-year-old boy in a school football match. He faints suddenly on the field. While everyone assumes it’s dehydration, later evaluation reveals hypertrophic cardiomyopathy (HCM) — a condition that thickens the heart muscle. If caught earlier, this risk could have been managed with monitoring and activity restrictions.
This is the reason awareness campaigns are essential not just among parents, but also teachers, coaches, and healthcare providers.
Types of Cardiomyopathy Conditions in Children
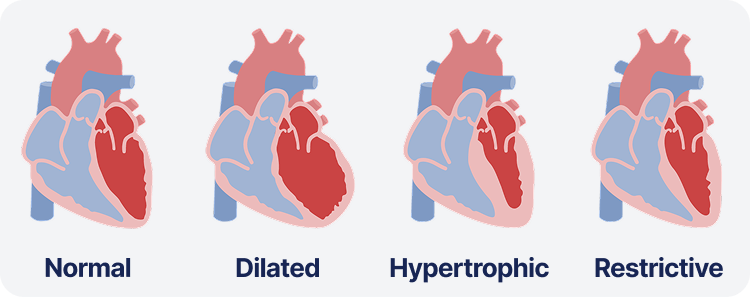
There are three main types of cardiomyopathy conditions seen in children. Knowing each of them well is better as it requires a different approach to care.
1. Dilated Cardiomyopathy (DCM)
This is the most common type found in children. In dilated cardiomyopathy, the heart muscle becomes weak and stretched, which reduces the ability of the heart to pump blood efficiently. Children with DCM may appear unusually tired, may struggle with feeding, or may have trouble gaining weight. In severe cases, it can lead to heart failure.
2. Hypertrophic Cardiomyopathy (HCM)
In hypertrophic cardiomyopathy, the heart muscle becomes abnormally thick. While it may not always cause symptoms, it can make it harder for the heart to relax and fill with blood. This condition is sometimes linked with sudden cardiac arrest in young athletes, making it particularly concerning.
3. Restrictive Cardiomyopathy (RCM)
This is one of the rarest types in children. In restrictive cardiomyopathy, the heart muscle becomes stiff, making it difficult for the heart to fill properly with blood. As a result, the heart cannot supply the body with enough oxygen, which can cause fatigue, swelling, and difficulty breathing.
4. Other Rare Types of Cardiomyopathy in Children
There are other forms like arrhythmogenic right ventricular cardiomyopathy and left ventricular non-compaction. Although rare, they can still pose serious risks and require specialized medical attention.
Causes of Cardiomyopathy in Children
The causes vary widely and can be as follows:
- Genetic mutations (inherited conditions)
- Infections (viral myocarditis damaging the heart muscle)
- Metabolic or mitochondrial disorders
- Autoimmune diseases
- Toxin or chemotherapy exposure
- Unknown causes (idiopathic) – nearly half of cases, no clear reason found
Symptoms of Cardiomyopathy Every Parent Should Look For

The tricky part is that symptoms often mimic common childhood issues. Parents should be alert if their child shows:
- Fatigue or low energy
- Shortness of breath (especially during play or at night)
- Swelling in the legs, ankles, or abdomen
- Fainting spells or dizziness
- Rapid or irregular heartbeat
- Difficulty feeding (in infants)
- Poor growth or weight gain
These may or may not always mean heart disease, but if they persist or worsen, a pediatric cardiology evaluation is necessary.
Diagnosis: How Doctors Detect Cardiomyopathy in Children?
Diagnosing cardiomyopathy requires a combination of medical history, physical examination, and advanced tests.
Doctors may use echocardiograms, electrocardiograms (ECG), chest X-rays, or cardiac MRI to look closely at the heart’s structure and function. Genetic testing may also be recommended, especially if there is a family history of the condition.
Early diagnosis makes a difference. Children who are diagnosed in the early stages can often be managed with medications and lifestyle changes before the condition progresses to more severe outcomes.
Treatment Options Available for Cardiomyopathic Conditions in Children
Treatment depends on type and severity, but it usually involves a mix of:
Medications
Drugs may be prescribed to manage symptoms, improve heart function, or regulate heart rhythm. These include beta-blockers, ACE inhibitors, and diuretics.
Lifestyle Management
Adjustments in daily activities may be recommended, such as limiting strenuous exercise, following a healthy diet, and monitoring fluid intake.
Medical Devices
In severe cases, devices like pacemakers or implantable cardioverter defibrillators (ICDs) may be used to regulate heart rhythm and prevent sudden complications.
Surgery and Transplants
For children with advanced cardiomyopathy who do not respond to other treatments, surgery or heart transplantation may be necessary.
Prognosis: Living with Cardiomyopathy and Long-Term Care in Children
The long-term outlook for children with cardiomyopathy depends on the type, severity, and how early it is detected. Some children live relatively normal lives with regular monitoring and medications, while others may face more serious challenges.
Ongoing care is a must. Children with cardiomyopathy need regular check-ups, tests, and sometimes lifelong treatment. Emotional and psychological support for both the child and the family also plays an important role in long-term care.
The Role of AI & Healthtech in Pediatric Heart Care

Technology is reshaping how we detect and manage pediatric heart conditions:
- AI-powered ECG analysis can flag early arrhythmias.
- Wearables (like smartwatches) monitor heart rate and detect abnormalities.
- Remote monitoring apps help doctors track a child’s progress at home.
- Predictive analytics identify children at higher risk of CVD complications.
For rare diseases like cardiomyopathy, AI offers hope for faster diagnosis, personalized treatment, and better long-term outcomes.
Raising Awareness: What Parents Can Do to Support Children with Cardiomyopathy?
According to the Pediatric Cardiomyopathy Registry (PCMR), about 1 in 100,000 children are diagnosed with cardiomyopathy each year worldwide.
- Know the symptoms and seek early evaluation.
- Share family medical history. Many cases are genetic.
- Join support groups to connect with other families.
- Advocate for better healthcare access especially in underserved communities.
- Encourage healthy routines: balanced diet, safe activity, regular check-ups.
Awareness campaigns and conversations reduce stigma and ensure that no child suffers in silence.
Protecting Little Hearts for a Better Future!
Cardiomyopathy in children is rare, but its impact is profound. From genetic inheritance to environmental triggers, it can silently affect young hearts, often without warning.
Helius Wellness strongly believes that with early diagnosis, advanced treatment, and parental awareness, many children can live healthier, fuller lives.
Technology, AI, and community awareness add another layer of hope, ensuring that families don’t feel alone in this fight.
Every child deserves a strong, healthy heart and together, we can make that possible.
India’s first AI-powered NCD diagnostics network.
Helius Wellness 2026. All Rights Reserved
May 27, 2025
Alcohol and Heart Health: The Rise of AI in Addiction Treatment
Alcohol quietly harms the heart over time, raising blood pressure, weakening heart muscles, and increasing the risk of failure, even at so‑called “moderate” levels of drinking. With AI‑powered diagnostics, wearables, and personalized support, Helius Wellness helps detect risks early and guide smarter, more effective addiction treatment for long‑term heart health.
Author:
Paresh Masani
Though adults are usually the focus when we talk about heart disease, children can also face serious heart conditions. Childhood heart problems are rare, and congenital heart defects (CHD) often come to mind first. But cardiomyopathy is another serious condition that affects children.
Cardiomyopathy impacts the heart muscle, making it harder for the heart to pump blood properly. While it may not be as commonly discussed as CHD, it can have serious consequences for growth, development, and overall well-being. The challenge is that many families do not realize that young children may also face such conditions, which means diagnosis is often delayed.
By spreading awareness, offering clear information, and supporting parents with the right resources, we can help ensure children with cardiomyopathy receive care at the earliest stage possible. Early conversations about this condition open the door to better health outcomes and stronger support systems for families.
What is Cardiomyopathy in Children?
Cardiomyopathy is a disease of the heart muscle that reduces its ability to pump blood efficiently. Over time, this weakness or stiffness in the heart muscle can lead to heart failure, life-threatening arrhythmias, or even sudden cardiac arrest.
Unlike adult heart disease, which is often linked to lifestyle factors like smoking, obesity, or diabetes, cardiomyopathy in children is more often associated with genetic factors, infections, or underlying medical conditions.
Why Awareness of Cardiomyopathies is So Important?
Unlike congenital heart defects (CHD), which are often detected soon after birth, cardiomyopathy can develop months or even years later. This makes it trickier to spot, and many children don’t show obvious symptoms until the condition has progressed.
Reasons awareness is important:
- Silent progression: A child may appear healthy but still have underlying heart muscle weakness.
- Misdiagnosis risk: Fatigue, poor appetite, or fainting might be mistaken for minor health issues or even “laziness.
- High-risk outcomes: Cardiomyopathy is a leading cause of sudden cardiac death in young athletes. Many tragic incidents reported globally, including in India, involve children collapsing during school sports.
- Better prognosis with early care: When diagnosed early, many children can manage the disease with medication and lifestyle changes, avoiding severe complications.
Imagine a 10-year-old boy in a school football match. He faints suddenly on the field. While everyone assumes it’s dehydration, later evaluation reveals hypertrophic cardiomyopathy (HCM) — a condition that thickens the heart muscle. If caught earlier, this risk could have been managed with monitoring and activity restrictions.
This is the reason awareness campaigns are essential not just among parents, but also teachers, coaches, and healthcare providers.
Types of Cardiomyopathy Conditions in Children

There are three main types of cardiomyopathy conditions seen in children. Knowing each of them well is better as it requires a different approach to care.
1. Dilated Cardiomyopathy (DCM)
This is the most common type found in children. In dilated cardiomyopathy, the heart muscle becomes weak and stretched, which reduces the ability of the heart to pump blood efficiently. Children with DCM may appear unusually tired, may struggle with feeding, or may have trouble gaining weight. In severe cases, it can lead to heart failure.
2. Hypertrophic Cardiomyopathy (HCM)
In hypertrophic cardiomyopathy, the heart muscle becomes abnormally thick. While it may not always cause symptoms, it can make it harder for the heart to relax and fill with blood. This condition is sometimes linked with sudden cardiac arrest in young athletes, making it particularly concerning.
3. Restrictive Cardiomyopathy (RCM)
This is one of the rarest types in children. In restrictive cardiomyopathy, the heart muscle becomes stiff, making it difficult for the heart to fill properly with blood. As a result, the heart cannot supply the body with enough oxygen, which can cause fatigue, swelling, and difficulty breathing.
4. Other Rare Types of Cardiomyopathy in Children
There are other forms like arrhythmogenic right ventricular cardiomyopathy and left ventricular non-compaction. Although rare, they can still pose serious risks and require specialized medical attention.
Causes of Cardiomyopathy in Children
The causes vary widely and can be as follows:
- Genetic mutations (inherited conditions)
- Infections (viral myocarditis damaging the heart muscle)
- Metabolic or mitochondrial disorders
- Autoimmune diseases
- Toxin or chemotherapy exposure
- Unknown causes (idiopathic) – nearly half of cases, no clear reason found
Symptoms of Cardiomyopathy Every Parent Should Look For

The tricky part is that symptoms often mimic common childhood issues. Parents should be alert if their child shows:
- Fatigue or low energy
- Shortness of breath (especially during play or at night)
- Swelling in the legs, ankles, or abdomen
- Fainting spells or dizziness
- Rapid or irregular heartbeat
- Difficulty feeding (in infants)
- Poor growth or weight gain
These may or may not always mean heart disease, but if they persist or worsen, a pediatric cardiology evaluation is necessary.
Diagnosis: How Doctors Detect Cardiomyopathy in Children?
Diagnosing cardiomyopathy requires a combination of medical history, physical examination, and advanced tests.
Doctors may use echocardiograms, electrocardiograms (ECG), chest X-rays, or cardiac MRI to look closely at the heart’s structure and function. Genetic testing may also be recommended, especially if there is a family history of the condition.
Early diagnosis makes a difference. Children who are diagnosed in the early stages can often be managed with medications and lifestyle changes before the condition progresses to more severe outcomes.
Treatment Options Available for Cardiomyopathic Conditions in Children
Treatment depends on type and severity, but it usually involves a mix of:
Medications
Drugs may be prescribed to manage symptoms, improve heart function, or regulate heart rhythm. These include beta-blockers, ACE inhibitors, and diuretics.
Lifestyle Management
Adjustments in daily activities may be recommended, such as limiting strenuous exercise, following a healthy diet, and monitoring fluid intake.
Medical Devices
In severe cases, devices like pacemakers or implantable cardioverter defibrillators (ICDs) may be used to regulate heart rhythm and prevent sudden complications.
Surgery and Transplants
For children with advanced cardiomyopathy who do not respond to other treatments, surgery or heart transplantation may be necessary.
Prognosis: Living with Cardiomyopathy and Long-Term Care in Children
The long-term outlook for children with cardiomyopathy depends on the type, severity, and how early it is detected. Some children live relatively normal lives with regular monitoring and medications, while others may face more serious challenges.
Ongoing care is a must. Children with cardiomyopathy need regular check-ups, tests, and sometimes lifelong treatment. Emotional and psychological support for both the child and the family also plays an important role in long-term care.
The Role of AI & Healthtech in Pediatric Heart Care

Technology is reshaping how we detect and manage pediatric heart conditions:
- AI-powered ECG analysis can flag early arrhythmias.
- Wearables (like smartwatches) monitor heart rate and detect abnormalities.
- Remote monitoring apps help doctors track a child’s progress at home.
- Predictive analytics identify children at higher risk of CVD complications.
For rare diseases like cardiomyopathy, AI offers hope for faster diagnosis, personalized treatment, and better long-term outcomes.
Raising Awareness: What Parents Can Do to Support Children with Cardiomyopathy?
According to the Pediatric Cardiomyopathy Registry (PCMR), about 1 in 100,000 children are diagnosed with cardiomyopathy each year worldwide.
- Know the symptoms and seek early evaluation.
- Share family medical history. Many cases are genetic.
- Join support groups to connect with other families.
- Advocate for better healthcare access especially in underserved communities.
- Encourage healthy routines: balanced diet, safe activity, regular check-ups.
Awareness campaigns and conversations reduce stigma and ensure that no child suffers in silence.
Protecting Little Hearts for a Better Future!
Cardiomyopathy in children is rare, but its impact is profound. From genetic inheritance to environmental triggers, it can silently affect young hearts, often without warning.
Helius Wellness strongly believes that with early diagnosis, advanced treatment, and parental awareness, many children can live healthier, fuller lives.
Technology, AI, and community awareness add another layer of hope, ensuring that families don’t feel alone in this fight.
Every child deserves a strong, healthy heart and together, we can make that possible.
India’s first AI-powered NCD diagnostics network.
May 27, 2025
Alcohol and Heart Health: The Rise of AI in Addiction Treatment
Alcohol quietly harms the heart over time, raising blood pressure, weakening heart muscles, and increasing the risk of failure, even at so‑called “moderate” levels of drinking. With AI‑powered diagnostics, wearables, and personalized support, Helius Wellness helps detect risks early and guide smarter, more effective addiction treatment for long‑term heart health.
Author:
Paresh Masani
Alcohol may feel like a common part of everyday life. It’s found in social gatherings, celebrations, and even as a way to relax after a long day. Apart from the cultural acceptance, alcohol can quietly and consistently damage the heart. The long-term effects of alcohol use like a rise in blood pressure and risk of heart failure are serious. When drinking becomes excessive or an addiction causes Alcohol Use Disorder (AUD), a condition that impacts not just the body, but also mental and emotional well-being.
The good news? Technology advances in Artificial Intelligence (AI) and wearable health tech bring an era of early detection, personalized support, and preventive care. This blog post takes a close look at how alcohol affects heart health and how AI is offering new hope in addiction treatment.
How Much Alcohol is Too Much for Your Heart?
There’s been a long-standing belief that moderate drinking, especially red wine, might be good for the heart. Some studies have shown benefits like slightly higher levels of HDL ("good") cholesterol. But recent research says the risks far outweigh any minor benefits. Even small amounts of alcohol can raise your blood pressure, trigger inflammation, and disrupt normal heart rhythms.
The World Health Organization now says there’s no safe level of alcohol use. Regular consumption in small amounts can quietly cause damage. Heavy drinking increases the risk of conditions like:
- High blood pressure
- Cardiomyopathy (weakened heart muscle)
- Arrhythmias (irregular heartbeats)
- Sudden cardiac death
The effects are especially severe when alcohol use is consistent over months or years.
Medical Advice: What’s Safe for Alcohol?
Doctors increasingly advise avoiding alcohol altogether, especially for those with heart conditions, high blood pressure, or diabetes. If you do drink, the key is moderation:
- No more than 1 drink per day for women
- No more than 2 drinks per day for men
- Avoid binge drinking (4+ drinks in 2 hours for women, 5+ for men)
Binge drinking can cause dangerous spikes in heart rate and blood pressure. Even occasional overuse can trigger arrhythmias or strokes.
Alcohol and Surgery: A Risky Combination
Before any surgery, especially involving the heart, doctors want to know about your alcohol use. That’s because alcohol interferes with how your body responds to anesthesia and stress. It can increase the risk of infection, delay healing, and raise the chance of complications like abnormal heart rhythms during and after the procedure.
Health experts recommend reducing or stopping alcohol intake several weeks before surgery to improve recovery outcomes. Patients who drink heavily have a higher likelihood of post-surgical problems, and understanding alcohol’s impact can help healthcare providers better prepare and monitor the patient.
How Alcohol Slowly Damages the Heart?
Alcohol might not seem dangerous at first. But even without obvious symptoms, it can gradually harm your cardiovascular system. Here’s how:
- Raises blood pressure: Alcohol tightens blood vessels, forcing the heart to pump harder.
- Disrupts heart rhythm: It interferes with the electrical signals that regulate your heartbeat.
- Elevates triglycerides: Alcohol raises levels of unhealthy fats in the blood, leading to artery blockages.
- Weakens heart muscle: Over time, the constant strain can lead to cardiomyopathy.
The effect? Higher risk of heart attacks, strokes, and heart failure.
Alcohol’s Link to High Blood Pressure
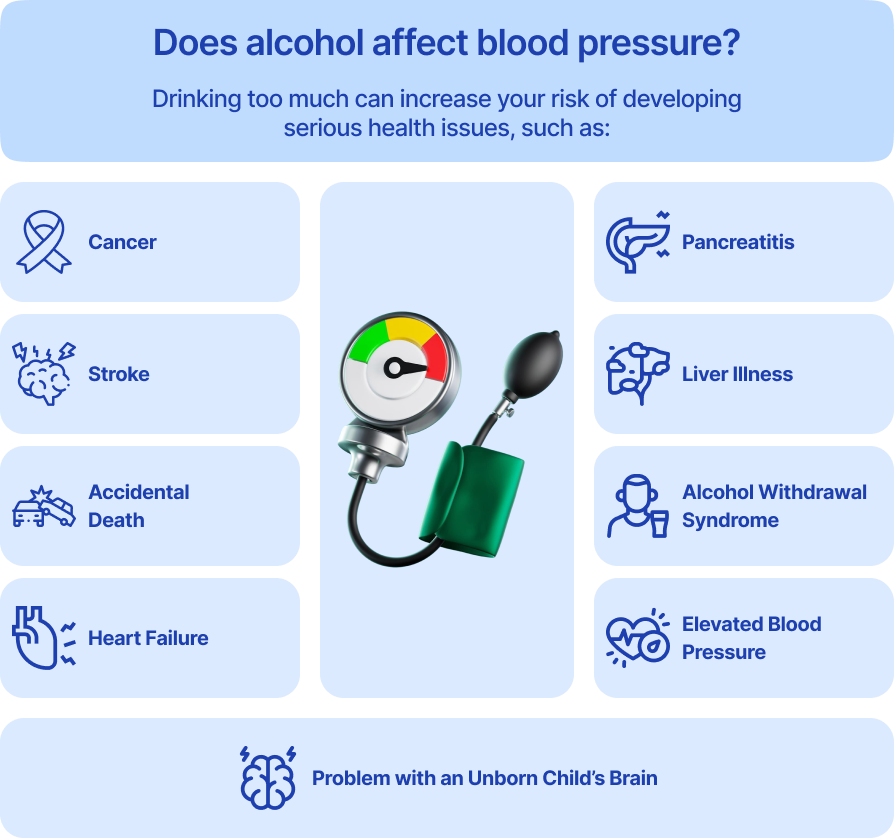
Alcohol is a known contributor to long-term high blood pressure. It acts on multiple systems in the body:
- Constriction of blood vessels
- Increased fluid in the bloodstream
- Surge in stress hormones like cortisol
All of these put extra strain on the cardiovascular system, increasing the risk of heart and kidney damage. Studies show that people who drink regularly are more likely to develop hypertension, especially if they have other risk factors like poor diet or a sedentary lifestyle.
Did You Know About Alcohol Use Disorder (AUD)?
AUD is a chronic brain condition where a person is unable to stop or control their drinking despite negative consequences. It usually develops over time:
Stage 1: Occasional social drinking
Stage 2: Increased reliance on stress relief or sleep
Stage 3: Tolerance and dependence
Eventually, alcohol becomes a coping mechanism, and quitting can cause withdrawal symptoms like anxiety, nausea, and tremors. AUD often affects emotional health, family life, and work performance.
What Actually Triggers Alcohol Addiction?
Common triggers that lead to alcohol misuse include:
- Chronic stress
- Trauma or mental health issues (depression, anxiety)
- Social pressure
- Family history of addiction
- Lack of support systems
Once alcohol becomes a primary coping tool, it becomes difficult to stop without external help. This is why early intervention and support matter.
The Impact of Alcohol Addiction on the Heart
Alcohol addiction does more than harm the liver—it deeply affects cardiovascular health:
- Increases the risk of atrial fibrillation
- Weakens the heart muscle (dilated cardiomyopathy)
- Leads to persistent hypertension
- Raises the risk of stroke and sudden cardiac death
Addiction also leads to irregular self-care. People may neglect medication, skip doctor visits, or eat unhealthy diets, worsening their heart condition.
How AI Is Changing Addiction Treatment?
Traditional addiction care often focuses on in-person therapy, rehab programs, or support groups. But AI is now making care more proactive, personal, and accessible. Here’s how:
- Early detection:AI analyzes speech, behavior, sleep patterns, and social activity to detect signs of addiction.
- Continuous monitoring:AI-powered Wearable devices track heart rate, stress, and sleep to spot early warning signs of relapse.
- Personalized support:Apps use machine learning to offer tips, reminders, and interventions tailored to the user’s needs.
AI systems help intervene before a person hits a crisis point, offering care that's always on and always adapting.
Examples of AI Tools Supporting Recovery
Some real-world solutions already helping with alcohol addiction include:
- Sober Grid:A peer support app with AI-driven relapse prediction.
- Vorvida:An interactive coaching platform that offers cognitive behavioral tools.
- RecoveryAI:Uses behavioral data to alert care teams of early relapse signs.
- CleverCare:Monitors vitals and mood data from wearables to optimize treatment.
These tools provide support anytime, anywhere—especially useful for people who live in remote areas or want privacy.
AI Brings More Inclusive and Fair Health Care
AI also helps make treatment more inclusive:
- Smart matching:Platforms match patients with culturally appropriate therapists
- Bias reduction:Tools like Textio and Pymetrics help clinics identify and fix inequalities in hiring and care
- Language support:AI tools can offer multilingual therapy or resources, broadening access for underserved populations
Means more people get the kind of care that fits their background, preferences, and values.
Bringing AI into Clinics and Wellness Programs
Healthcare providers can start integrating AI by:
- Using screening tools that flag early warning signs of addiction
- Adding wearable devices to monitor stress and heart health
- Offering digital support apps that provide 24/7 care
- Training staff with AI to personalize treatment plans
These steps not only improve recovery outcomes but also help prevent irreversible damage to the heart.
Protecting Heart Health by Addressing Alcohol Early!
Alcohol may feel like a small part of life, but its effects on the heart are anything but small. Over time, drinking can raise blood pressure, cause heart rhythm issues, and lead to heart failure. But we’re no longer limited to traditional care models.
Helius Wellness believes in catching problems early and empowering patients through smart, tech-driven care. AI tools and wearable devices are bringing prevention and recovery into everyday life, helping people survive and thrive.
The future of heart health starts with early intervention, and the power of AI is making that future a reality.
India’s first AI-powered NCD diagnostics network.