July 16, 2025
CVD Risks in Women and Children: Why Preventive Care Matters?
Protect women and children from often-overlooked heart risks with early screening, lifestyle changes, and AI-powered preventive care tailored for Indian families.
Author:
Kavya Dave
Though adults are usually the focus when we talk about heart disease, children can also face serious heart conditions. Childhood heart problems are rare, and congenital heart defects (CHD) often come to mind first. But cardiomyopathy is another serious condition that affects children.
Cardiomyopathy impacts the heart muscle, making it harder for the heart to pump blood properly. While it may not be as commonly discussed as CHD, it can have serious consequences for growth, development, and overall well-being. The challenge is that many families do not realize that young children may also face such conditions, which means diagnosis is often delayed.
By spreading awareness, offering clear information, and supporting parents with the right resources, we can help ensure children with cardiomyopathy receive care at the earliest stage possible. Early conversations about this condition open the door to better health outcomes and stronger support systems for families.
What is Cardiomyopathy in Children?
Cardiomyopathy is a disease of the heart muscle that reduces its ability to pump blood efficiently. Over time, this weakness or stiffness in the heart muscle can lead to heart failure, life-threatening arrhythmias, or even sudden cardiac arrest.
Unlike adult heart disease, which is often linked to lifestyle factors like smoking, obesity, or diabetes, cardiomyopathy in children is more often associated with genetic factors, infections, or underlying medical conditions.
Why Awareness of Cardiomyopathies is So Important?
Unlike congenital heart defects (CHD), which are often detected soon after birth, cardiomyopathy can develop months or even years later. This makes it trickier to spot, and many children don’t show obvious symptoms until the condition has progressed.
Reasons awareness is important:
- Silent progression: A child may appear healthy but still have underlying heart muscle weakness.
- Misdiagnosis risk: Fatigue, poor appetite, or fainting might be mistaken for minor health issues or even “laziness.
- High-risk outcomes: Cardiomyopathy is a leading cause of sudden cardiac death in young athletes. Many tragic incidents reported globally, including in India, involve children collapsing during school sports.
- Better prognosis with early care: When diagnosed early, many children can manage the disease with medication and lifestyle changes, avoiding severe complications.
Imagine a 10-year-old boy in a school football match. He faints suddenly on the field. While everyone assumes it’s dehydration, later evaluation reveals hypertrophic cardiomyopathy (HCM) — a condition that thickens the heart muscle. If caught earlier, this risk could have been managed with monitoring and activity restrictions.
This is the reason awareness campaigns are essential not just among parents, but also teachers, coaches, and healthcare providers.
Types of Cardiomyopathy Conditions in Children
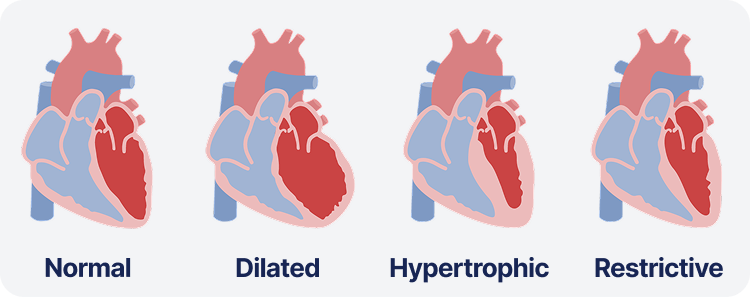
There are three main types of cardiomyopathy conditions seen in children. Knowing each of them well is better as it requires a different approach to care.
1. Dilated Cardiomyopathy (DCM)
This is the most common type found in children. In dilated cardiomyopathy, the heart muscle becomes weak and stretched, which reduces the ability of the heart to pump blood efficiently. Children with DCM may appear unusually tired, may struggle with feeding, or may have trouble gaining weight. In severe cases, it can lead to heart failure.
2. Hypertrophic Cardiomyopathy (HCM)
In hypertrophic cardiomyopathy, the heart muscle becomes abnormally thick. While it may not always cause symptoms, it can make it harder for the heart to relax and fill with blood. This condition is sometimes linked with sudden cardiac arrest in young athletes, making it particularly concerning.
3. Restrictive Cardiomyopathy (RCM)
This is one of the rarest types in children. In restrictive cardiomyopathy, the heart muscle becomes stiff, making it difficult for the heart to fill properly with blood. As a result, the heart cannot supply the body with enough oxygen, which can cause fatigue, swelling, and difficulty breathing.
4. Other Rare Types of Cardiomyopathy in Children
There are other forms like arrhythmogenic right ventricular cardiomyopathy and left ventricular non-compaction. Although rare, they can still pose serious risks and require specialized medical attention.
Causes of Cardiomyopathy in Children
The causes vary widely and can be as follows:
- Genetic mutations (inherited conditions)
- Infections (viral myocarditis damaging the heart muscle)
- Metabolic or mitochondrial disorders
- Autoimmune diseases
- Toxin or chemotherapy exposure
- Unknown causes (idiopathic) – nearly half of cases, no clear reason found
Symptoms of Cardiomyopathy Every Parent Should Look For

The tricky part is that symptoms often mimic common childhood issues. Parents should be alert if their child shows:
- Fatigue or low energy
- Shortness of breath (especially during play or at night)
- Swelling in the legs, ankles, or abdomen
- Fainting spells or dizziness
- Rapid or irregular heartbeat
- Difficulty feeding (in infants)
- Poor growth or weight gain
These may or may not always mean heart disease, but if they persist or worsen, a pediatric cardiology evaluation is necessary.
Diagnosis: How Doctors Detect Cardiomyopathy in Children?
Diagnosing cardiomyopathy requires a combination of medical history, physical examination, and advanced tests.
Doctors may use echocardiograms, electrocardiograms (ECG), chest X-rays, or cardiac MRI to look closely at the heart’s structure and function. Genetic testing may also be recommended, especially if there is a family history of the condition.
Early diagnosis makes a difference. Children who are diagnosed in the early stages can often be managed with medications and lifestyle changes before the condition progresses to more severe outcomes.
Treatment Options Available for Cardiomyopathic Conditions in Children
Treatment depends on type and severity, but it usually involves a mix of:
Medications
Drugs may be prescribed to manage symptoms, improve heart function, or regulate heart rhythm. These include beta-blockers, ACE inhibitors, and diuretics.
Lifestyle Management
Adjustments in daily activities may be recommended, such as limiting strenuous exercise, following a healthy diet, and monitoring fluid intake.
Medical Devices
In severe cases, devices like pacemakers or implantable cardioverter defibrillators (ICDs) may be used to regulate heart rhythm and prevent sudden complications.
Surgery and Transplants
For children with advanced cardiomyopathy who do not respond to other treatments, surgery or heart transplantation may be necessary.
Prognosis: Living with Cardiomyopathy and Long-Term Care in Children
The long-term outlook for children with cardiomyopathy depends on the type, severity, and how early it is detected. Some children live relatively normal lives with regular monitoring and medications, while others may face more serious challenges.
Ongoing care is a must. Children with cardiomyopathy need regular check-ups, tests, and sometimes lifelong treatment. Emotional and psychological support for both the child and the family also plays an important role in long-term care.
The Role of AI & Healthtech in Pediatric Heart Care

Technology is reshaping how we detect and manage pediatric heart conditions:
- AI-powered ECG analysis can flag early arrhythmias.
- Wearables (like smartwatches) monitor heart rate and detect abnormalities.
- Remote monitoring apps help doctors track a child’s progress at home.
- Predictive analytics identify children at higher risk of CVD complications.
For rare diseases like cardiomyopathy, AI offers hope for faster diagnosis, personalized treatment, and better long-term outcomes.
Raising Awareness: What Parents Can Do to Support Children with Cardiomyopathy?
According to the Pediatric Cardiomyopathy Registry (PCMR), about 1 in 100,000 children are diagnosed with cardiomyopathy each year worldwide.
- Know the symptoms and seek early evaluation.
- Share family medical history. Many cases are genetic.
- Join support groups to connect with other families.
- Advocate for better healthcare access especially in underserved communities.
- Encourage healthy routines: balanced diet, safe activity, regular check-ups.
Awareness campaigns and conversations reduce stigma and ensure that no child suffers in silence.
Protecting Little Hearts for a Better Future!
Cardiomyopathy in children is rare, but its impact is profound. From genetic inheritance to environmental triggers, it can silently affect young hearts, often without warning.
Helius Wellness strongly believes that with early diagnosis, advanced treatment, and parental awareness, many children can live healthier, fuller lives.
Technology, AI, and community awareness add another layer of hope, ensuring that families don’t feel alone in this fight.
Every child deserves a strong, healthy heart and together, we can make that possible.
India’s first AI-powered NCD diagnostics network.
Helius Wellness 2026. All Rights Reserved
July 16, 2025
CVD Risks in Women and Children: Why Preventive Care Matters?
Protect women and children from often-overlooked heart risks with early screening, lifestyle changes, and AI-powered preventive care tailored for Indian families.
Author:
Kavya Dave
Though adults are usually the focus when we talk about heart disease, children can also face serious heart conditions. Childhood heart problems are rare, and congenital heart defects (CHD) often come to mind first. But cardiomyopathy is another serious condition that affects children.
Cardiomyopathy impacts the heart muscle, making it harder for the heart to pump blood properly. While it may not be as commonly discussed as CHD, it can have serious consequences for growth, development, and overall well-being. The challenge is that many families do not realize that young children may also face such conditions, which means diagnosis is often delayed.
By spreading awareness, offering clear information, and supporting parents with the right resources, we can help ensure children with cardiomyopathy receive care at the earliest stage possible. Early conversations about this condition open the door to better health outcomes and stronger support systems for families.
What is Cardiomyopathy in Children?
Cardiomyopathy is a disease of the heart muscle that reduces its ability to pump blood efficiently. Over time, this weakness or stiffness in the heart muscle can lead to heart failure, life-threatening arrhythmias, or even sudden cardiac arrest.
Unlike adult heart disease, which is often linked to lifestyle factors like smoking, obesity, or diabetes, cardiomyopathy in children is more often associated with genetic factors, infections, or underlying medical conditions.
Why Awareness of Cardiomyopathies is So Important?
Unlike congenital heart defects (CHD), which are often detected soon after birth, cardiomyopathy can develop months or even years later. This makes it trickier to spot, and many children don’t show obvious symptoms until the condition has progressed.
Reasons awareness is important:
- Silent progression: A child may appear healthy but still have underlying heart muscle weakness.
- Misdiagnosis risk: Fatigue, poor appetite, or fainting might be mistaken for minor health issues or even “laziness.
- High-risk outcomes: Cardiomyopathy is a leading cause of sudden cardiac death in young athletes. Many tragic incidents reported globally, including in India, involve children collapsing during school sports.
- Better prognosis with early care: When diagnosed early, many children can manage the disease with medication and lifestyle changes, avoiding severe complications.
Imagine a 10-year-old boy in a school football match. He faints suddenly on the field. While everyone assumes it’s dehydration, later evaluation reveals hypertrophic cardiomyopathy (HCM) — a condition that thickens the heart muscle. If caught earlier, this risk could have been managed with monitoring and activity restrictions.
This is the reason awareness campaigns are essential not just among parents, but also teachers, coaches, and healthcare providers.
Types of Cardiomyopathy Conditions in Children

There are three main types of cardiomyopathy conditions seen in children. Knowing each of them well is better as it requires a different approach to care.
1. Dilated Cardiomyopathy (DCM)
This is the most common type found in children. In dilated cardiomyopathy, the heart muscle becomes weak and stretched, which reduces the ability of the heart to pump blood efficiently. Children with DCM may appear unusually tired, may struggle with feeding, or may have trouble gaining weight. In severe cases, it can lead to heart failure.
2. Hypertrophic Cardiomyopathy (HCM)
In hypertrophic cardiomyopathy, the heart muscle becomes abnormally thick. While it may not always cause symptoms, it can make it harder for the heart to relax and fill with blood. This condition is sometimes linked with sudden cardiac arrest in young athletes, making it particularly concerning.
3. Restrictive Cardiomyopathy (RCM)
This is one of the rarest types in children. In restrictive cardiomyopathy, the heart muscle becomes stiff, making it difficult for the heart to fill properly with blood. As a result, the heart cannot supply the body with enough oxygen, which can cause fatigue, swelling, and difficulty breathing.
4. Other Rare Types of Cardiomyopathy in Children
There are other forms like arrhythmogenic right ventricular cardiomyopathy and left ventricular non-compaction. Although rare, they can still pose serious risks and require specialized medical attention.
Causes of Cardiomyopathy in Children
The causes vary widely and can be as follows:
- Genetic mutations (inherited conditions)
- Infections (viral myocarditis damaging the heart muscle)
- Metabolic or mitochondrial disorders
- Autoimmune diseases
- Toxin or chemotherapy exposure
- Unknown causes (idiopathic) – nearly half of cases, no clear reason found
Symptoms of Cardiomyopathy Every Parent Should Look For

The tricky part is that symptoms often mimic common childhood issues. Parents should be alert if their child shows:
- Fatigue or low energy
- Shortness of breath (especially during play or at night)
- Swelling in the legs, ankles, or abdomen
- Fainting spells or dizziness
- Rapid or irregular heartbeat
- Difficulty feeding (in infants)
- Poor growth or weight gain
These may or may not always mean heart disease, but if they persist or worsen, a pediatric cardiology evaluation is necessary.
Diagnosis: How Doctors Detect Cardiomyopathy in Children?
Diagnosing cardiomyopathy requires a combination of medical history, physical examination, and advanced tests.
Doctors may use echocardiograms, electrocardiograms (ECG), chest X-rays, or cardiac MRI to look closely at the heart’s structure and function. Genetic testing may also be recommended, especially if there is a family history of the condition.
Early diagnosis makes a difference. Children who are diagnosed in the early stages can often be managed with medications and lifestyle changes before the condition progresses to more severe outcomes.
Treatment Options Available for Cardiomyopathic Conditions in Children
Treatment depends on type and severity, but it usually involves a mix of:
Medications
Drugs may be prescribed to manage symptoms, improve heart function, or regulate heart rhythm. These include beta-blockers, ACE inhibitors, and diuretics.
Lifestyle Management
Adjustments in daily activities may be recommended, such as limiting strenuous exercise, following a healthy diet, and monitoring fluid intake.
Medical Devices
In severe cases, devices like pacemakers or implantable cardioverter defibrillators (ICDs) may be used to regulate heart rhythm and prevent sudden complications.
Surgery and Transplants
For children with advanced cardiomyopathy who do not respond to other treatments, surgery or heart transplantation may be necessary.
Prognosis: Living with Cardiomyopathy and Long-Term Care in Children
The long-term outlook for children with cardiomyopathy depends on the type, severity, and how early it is detected. Some children live relatively normal lives with regular monitoring and medications, while others may face more serious challenges.
Ongoing care is a must. Children with cardiomyopathy need regular check-ups, tests, and sometimes lifelong treatment. Emotional and psychological support for both the child and the family also plays an important role in long-term care.
The Role of AI & Healthtech in Pediatric Heart Care

Technology is reshaping how we detect and manage pediatric heart conditions:
- AI-powered ECG analysis can flag early arrhythmias.
- Wearables (like smartwatches) monitor heart rate and detect abnormalities.
- Remote monitoring apps help doctors track a child’s progress at home.
- Predictive analytics identify children at higher risk of CVD complications.
For rare diseases like cardiomyopathy, AI offers hope for faster diagnosis, personalized treatment, and better long-term outcomes.
Raising Awareness: What Parents Can Do to Support Children with Cardiomyopathy?
According to the Pediatric Cardiomyopathy Registry (PCMR), about 1 in 100,000 children are diagnosed with cardiomyopathy each year worldwide.
- Know the symptoms and seek early evaluation.
- Share family medical history. Many cases are genetic.
- Join support groups to connect with other families.
- Advocate for better healthcare access especially in underserved communities.
- Encourage healthy routines: balanced diet, safe activity, regular check-ups.
Awareness campaigns and conversations reduce stigma and ensure that no child suffers in silence.
Protecting Little Hearts for a Better Future!
Cardiomyopathy in children is rare, but its impact is profound. From genetic inheritance to environmental triggers, it can silently affect young hearts, often without warning.
Helius Wellness strongly believes that with early diagnosis, advanced treatment, and parental awareness, many children can live healthier, fuller lives.
Technology, AI, and community awareness add another layer of hope, ensuring that families don’t feel alone in this fight.
Every child deserves a strong, healthy heart and together, we can make that possible.
India’s first AI-powered NCD diagnostics network.
July 16, 2025
CVD Risks in Women and Children: Why Preventive Care Matters?
Protect women and children from often-overlooked heart risks with early screening, lifestyle changes, and AI-powered preventive care tailored for Indian families.
Author:
Kavya Dave
Cardiovascular disease (CVD) has long been misunderstood as something that mainly affects older men. This misconception has led to underdiagnosis, undertreatment, and a serious neglect of heart health in women and children.

In India, the reality is alarming. CVD is the leading cause of death among women, claiming nearly 800,000 lives annually before the age of 70. Childrens are affected more by congenital heart defects or lifestyle-related risks that are on the rise.
This blog brings attention to the often-overlooked heart health risks in women and children and explores the causes, warning signs, and why preventive care should be front and center.
Basic Understanding of CVD in Women and Children
Cardiovascular disease is not just an older adult problem. In women and children, it can present differently and too often it gets missed.
In women, CVD risk escalates after menopause due to the decline of estrogen, a hormone that offers some protection to the heart. Despite this, many women are not screened or treated in time.
Children may be born with congenital heart defects (CHDs) or develop problems later due to infections, poor nutrition, or sedentary lifestyles. Some conditions require surgery, but many can be managed if caught early.
The common thread? Subtle symptoms, underdiagnosis, and low awareness. Recognizing these patterns early can prevent long-term health issues and save lives.
Common Types of Heart Disease in Children and Teens
Many heart conditions in children go unnoticed until they cause serious complications. Here are the most common:
- Congenital Heart Defects (CHD): Structural problems like ventricular or atrial septal defects, hypoplastic left heart syndrome, and tetralogy of Fallot often need early surgical care.
- Arrhythmias: Irregular heartbeats like supraventricular tachycardia or bradycardia can cause dizziness or fainting and may require medication.
- Kawasaki Disease & Rheumatic Heart Disease: Inflammatory conditions linked to infections that can damage arteries or valves if not treated promptly.
- Atherosclerosis: Fat buildup in arteries can begin in childhood, especially in those with obesity or diabetes.
- Myocarditis, Pericarditis, and Heart Murmurs: These conditions may result from infections or underlying issues but are often manageable with timely care.
Early diagnosis and ongoing care can allow children with heart issues to lead full, active lives
The Growing Cardiovascular Burden in Indian Women
CVD is the number one killer of Indian women, responsible for nearly 800,000 deaths annually and more than half are premature.
Factors include:
- Rising obesity and abdominal fat
- High blood pressure and diabetes
- Increased tobacco use, particularly smokeless forms
- Hormonal shifts after menopause
- Low physical activity and poor dietary habits
Women also face cultural and systemic barriers like less access to healthcare, delayed diagnoses, and lower chances of receiving life-saving treatments. Bridging this gender gap requires both medical awareness and social change.
Hidden Risk Factors in Women and Children
Many risk factors for cardiovascular disease in women and children often go unnoticed, either because they don’t show early symptoms or because they're misunderstood. Recognizing these hidden risks is critical for prevention.
For Women:
- Hormonal Changes: After menopause, the drop in estrogen increases LDL cholesterol and blood pressure, elevating CVD risk.
- Mental Health: Anxiety, depression, and chronic stress can affect heart health, especially when left untreated.
- Social Bias: Women’s symptoms are often downplayed, leading to missed or delayed diagnoses.
For Children:
- Childhood Infections: Diseases like rheumatic fever and Kawasaki disease can silently damage heart valves and arteries.
- Poor Nutrition: High salt and sugar intake, often overlooked in daily snacks, contributes to early metabolic changes.
- Sedentary Habits: Screen-heavy routines and minimal physical activity are fueling obesity and hypertension in kids.
These subtle yet serious factors often escape early screenings and routine checkups. Awareness among parents, educators, and healthcare professionals helps identify and manage these risks before they lead to long-term heart problems.
Addressing Gaps in Awareness and Treatment
Heart disease in women and children remains underdiagnosed and undertreated. Key issues include:
- Low Awareness in Rural Areas: Hypertension awareness in rural women is just 25%, with only 1–6% having it under control.
- Lack of Regular Screenings: Routine checks for BP, cholesterol, and diabetes are still uncommon for younger women and adolescents.
- Healthcare Disparities: Women get fewer life-saving interventions and prescriptions. Children in low-income groups often lack access to diagnostics.
- Inadequate Training: Doctors often miss atypical symptoms in women and children, leading to delays in treatment.
To close these gaps, India needs community-based education, policy support, and better clinical training.
Actionable Steps to Improve Heart Health

Preventing heart disease in women and children is entirely possible with early and consistent actions. The goal is to combine awareness, screening, and better lifestyle choices with access to quality healthcare.
Here are steps we can take:
- Start Early: Introduce heart health education in schools and create awareness campaigns for adolescent girls and parents.
- Routine Screenings: Encourage annual blood pressure, cholesterol, and BMI checks for women and at-risk children.
- Physical Activity: Promote 30–60 minutes of daily movement through school programs and community efforts.
- Nutrition Awareness: Reduce processed foods and sugary drinks; increase fruits, vegetables, and fiber intake.
- Tobacco Control: Strengthen anti-tobacco education, especially in rural schools and among young women.
- Accessible Care: Improve access to medications, diagnostic tests, and emergency care in underserved areas.
- Empower with Information: Train healthcare providers to identify non-classic heart symptoms in women and kids.
These interventions don’t need high-cost infrastructure, they need strong intent, right policies, and consistent community engagement. When done right, these actions can help lower premature heart disease risk for generations.
The Role of AI and Digital Health in Preventive Cardiology
As healthcare systems look for scalable, early-stage interventions, Artificial Intelligence (AI) is emerging as a powerful ally in predicting and preventing cardiovascular disease, especially among high-risk groups like women and children.
AI for Early Detection
AI algorithms can analyze ECGs, wearable data, and medical histories to flag heart anomalies early even before symptoms appear. This is especially helpful in children with undiagnosed congenital issues or women with non-traditional heart attack symptoms.
Remote Monitoring and Wearables
Smart devices now track heart rate, blood pressure, and even irregular rhythms in real time. This data helps detect problems early and enables continuous care, especially for underserved areas where routine doctor visits are rare.
Personalized Risk Profiles
AI tools can assess individual risk by factoring in gender, age, family history, lifestyle, and biometrics. This helps tailor screening and prevention strategies for women and adolescents with subtle warning signs.
Decision Support for Doctors
Clinical decision-support tools powered by AI help doctors make faster, more accurate judgments about treatments, especially in emergency settings where women and children are often misdiagnosed.
In a country like India, where gaps in access and awareness are still wide, AI can make heart care more proactive, inclusive, and data-driven, bringing preventive care closer to those who need it most.
A Call to Action for Preventive Heart Health in Women and Children
Cardiovascular disease in women and children is a growing but preventable crisis. With rising premature deaths among women and early risk factors emerging in children, prevention must be a national priority.
Helius Wellness stresses the importance of early screenings, lifestyle education, equal access to care, and smarter use of technology like AI to change the future of heart health. It’s time we act!
Start early, stay aware, and prioritize the heart health of those often overlooked.
India’s first AI-powered NCD diagnostics network.